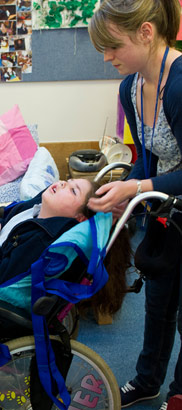
At birth, a baby has minimal control over voluntary movement. Neonatal reflexes are a survival strategy which disappear in the first 4-6 months, some being replaced by voluntary motor skills. In children with cerebral palsy some neonatal reflexes remain into adulthood, affecting the brain's control over basic movement patterns and postural reactions (eg balance).
For more information on early reflexes and disability click here.
The following slides focus on a motor development issue with cerebral palsy as the focus disability. This disability was chosen as it often co-occurs in children with CLDD. Background information about the motor developmental area can be found at Level B.

Cerebral palsy (CP) is the commonest cause of physical disability in childhood (UKCP, 2003). About 1 in 400 people are born with cerebral palsy, and 45% have intellectual impairment; 25% have severe learning difficulties (Scope, 2011).
All people with cerebral palsy have difficulties controlling movement and posture. They may experience:
- Involuntary movements (the severity depends on the form of cerebral palsy);
- Voluntary movement weakness or paralysis, causing slow movement initiation, difficulty in making discrete movements, mirroring or associated movements. (See: Abdel Rahman, 2011).
For possible associated difficulties, have a look at this list.

Children with cerebral palsy are not usually diagnosed until after the age of six months. Early signs include:
- Feeding difficulties (eg with sucking and swallowing) or lack of interest in food;
- Delayed smiling;
- Gaze differences;
- Increased, decreased or changing muscle tone;
- Irritability, anxiety, lack of interest in sounds or visual cues and sleep disturbance;
- Delayed postural and motor development;
- Assymetrical movement or tone;
- At four months, an inability to hold a stable head position, or bear weight on forearms.
(See: Abdel Rahman, 2011)
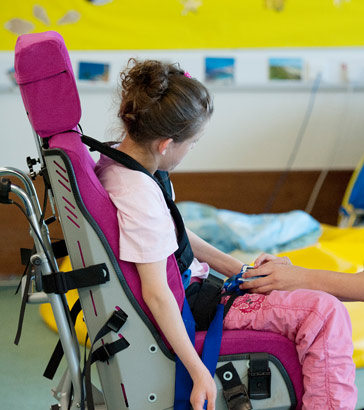
Activities that depend on gross and fine motor co-ordination skills (sitting, crawling, walking, running, manipulating
toys, feeding/drinking independently, etc.) increase a child's opportunities to find out about their world. Therefore, it
is important to bear in mind that any delay in motor development in the early years is likely to restrict cognitive development.
Alton, 2005

In children who have developmental brain lesions (eg cerebral palsy):
- Muscles do not develop normally;
- Bones do not develop tensile and compressive strength;
- The limited amount of movement causes a lack of development of neural connections or pathways in the brain.
(Damiano, 2008)
Cerebral palsy needs careful physical management to minimise the risk of secondary difficulties. Unless managed, muscle shortening, abnormal reflexes and static positioning can cause tissue contractures which in turn causes bones malformations (Abdel Raman, 2011).

Effective physical management requires families and a range of professionals including the physiotherapist, orthotist and occupational therapist to work together within an integrated therapy programme. The programme will aim to minimise secondary difficulties (eg contractures and bone deformities), maximise physical ability and function, and promote learning, communication and inclusion.

This may include:
- Correct positioning and postural management;
- An integrated therapy programme;
- Adaptive equipment (eg supported seating, standing frame, side lying board, wheelchair, sleep system);
- Orthotics (eg splints).
(See: Pountney, 2007)

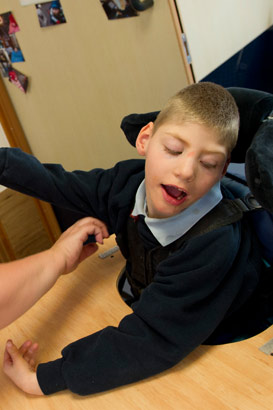
Educational practices for children with PMLD increasingly focus on functionality instead of developmental milestones. This is due to:
- The slow rate of development and learning;
- Development-focused intervention not impacting on functionality;
- Functional skills acquisition often exceeding the developmental milestones;
- Functional skills enhancing the child's independence and control over their own life.
Because of this shift towards a functional approach, motor assessment should also focus on functional skills and independence rather than developmental milestones.
(van der Putten et al, 2005)

- Patient/parent education on how to encourage more movement from infancy onward.
- Provide young patients with braces and mobility devices to promote activity.
- Develop specific therapeutic programmes with more intense levels of training to enhance activity levels.
- Explore recreational programmes in the community for more fun and long term fitness and health.
(Damiano, 2008)


Etzel-Wise, D. and Mears, B. (2004) Adapted physical education and therapeutic recreation in schools, Intervention
in School and Clinic, 39, 223-232.
Martin, S. (2006) Teaching Motor Skills to Children with Cerebral Palsy and Similar Movement Disorders: A guide for parents
and professionals. Bethesda, MD: Woodbine House.
Scope and Aspirico have jointly developed Celebrate Every Step, an online developmental recording system and play resource for young children with physical, sensory and learning needs.
There is more information on cerebral palsy in the neuroscience module of this learning resource.